Kennedy’s story: Navigating a rare heart defect with courage beyond her years
- Category: Cardiology, Patient Stories
- Posted on:

When Kim and Kyle Lord first learned they were pregnant in 2012, the couple was ecstatic to become first-time parents. Throughout Kim’s pregnancy, she was the picture of health, but as her due date approached, she developed preeclampsia and needed an emergency C-section for the safety of both herself and her baby. That day, a perfect little girl was born, whom the couple named Kennedy.
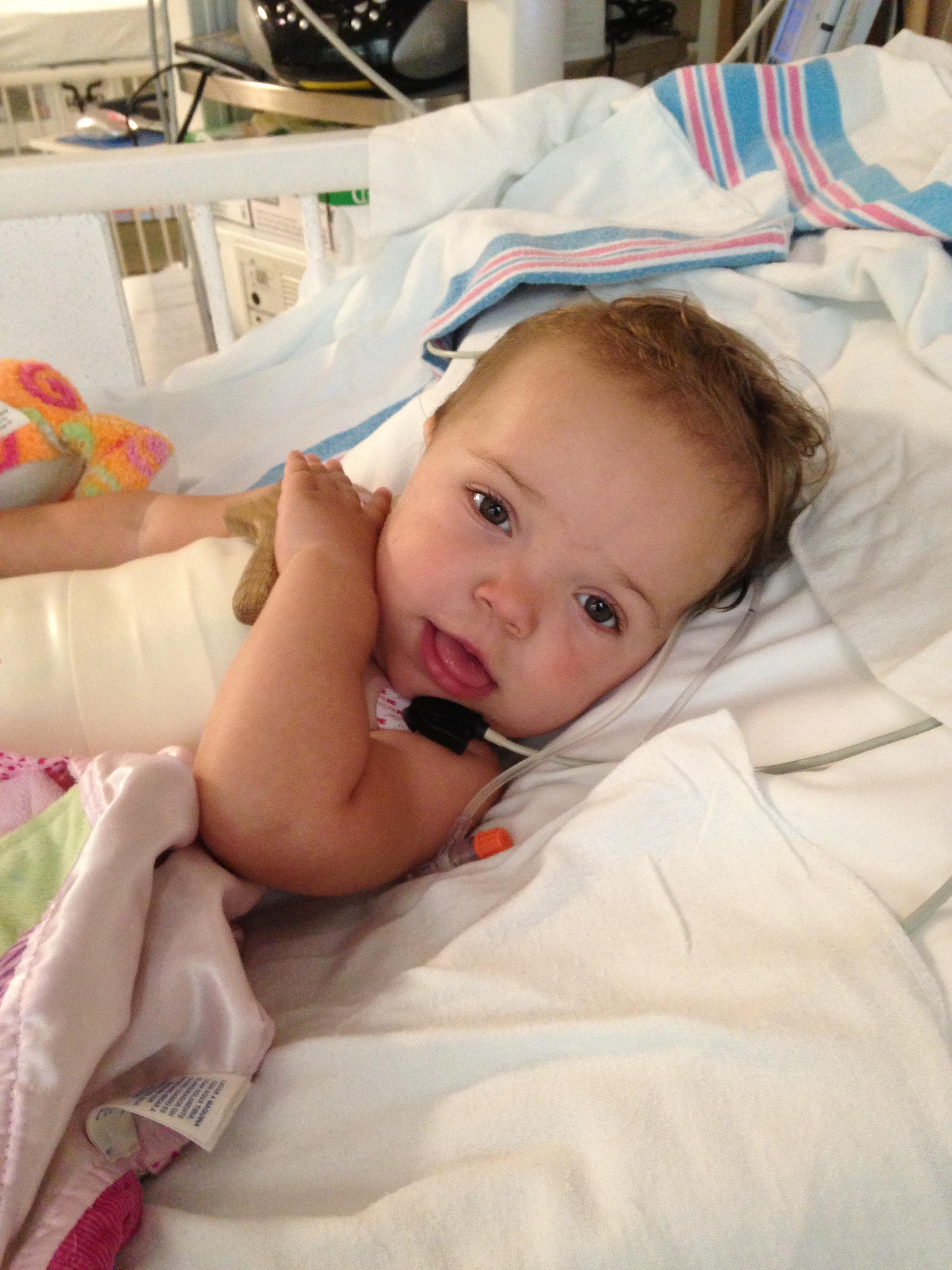 During the first months of her life, Kennedy remained extremely healthy and even managed to avoid most of the viruses that circulate throughout daycares and infect babies’ immature immune systems. But at 11 months old, a stomach bug finally caught up to her.
During the first months of her life, Kennedy remained extremely healthy and even managed to avoid most of the viruses that circulate throughout daycares and infect babies’ immature immune systems. But at 11 months old, a stomach bug finally caught up to her.
“I remember it clearly because we were on our way to daycare when she threw up all over the car seat,” Kim recalled. “So, we headed to the pediatrician instead that day.”
At the appointment, Kennedy’s doctor confirmed that she did, in fact, have a stomach bug—nothing to be too concerned about. But he also told Kim that during the examination, he heard a heart murmur through his stethoscope.
 “He didn’t want us to worry too much about it because he’d never detected a murmur in her before, and he said that it may have been related to her sickness,” Kim said. “Kennedy was already scheduled for another appointment a month later for her 12-month exam, so we decided he would just re-check at that time.”
“He didn’t want us to worry too much about it because he’d never detected a murmur in her before, and he said that it may have been related to her sickness,” Kim said. “Kennedy was already scheduled for another appointment a month later for her 12-month exam, so we decided he would just re-check at that time.”
But at the next appointment, her pediatrician could hear the heart murmur even more clearly than before.
"The murmur was significantly louder,” Kim said. “It was concerning enough for him to send her for an echocardiogram.”
The family went to a local hospital near their home in Alexandria, Louisiana for the echocardiogram, which uses ultrasound technology to produce a visual representation of how blood is moving through the heart. The test allows specialists to examine the structure and function of the heart’s chambers and valves, and it is the first major step in diagnosing heart conditions.
It was a test, and a day, the Lords will never forget. After the echocardiogram was completed, the pediatric cardiologist sat them down, and broke the news that their baby daughter had a severe heart defect that required surgery as soon as possible.
“It was shocking, and then just a whirlwind,” Kim said. “We had gone from thinking she was perfectly healthy with no issues to planning for an open-heart surgery.”
 The Lords were referred to The Heart Center at Children’s Hospital New Orleans, which provides comprehensive evaluation and treatment for patients with congenital cardiovascular disorders. It is the only facility in the state offering a comprehensive team of pediatric specialists and sub-specialists.
The Lords were referred to The Heart Center at Children’s Hospital New Orleans, which provides comprehensive evaluation and treatment for patients with congenital cardiovascular disorders. It is the only facility in the state offering a comprehensive team of pediatric specialists and sub-specialists.
The specialists at The Heart Center explained Kennedy’s diagnosis to the Lords in detail. Her disorder, called subaortic stenosis, involved the presence of a membrane that is akin to hardened muscle. That membrane exists just below the aortic valve, causing a blockage of blood flow at the left ventricle (the lower left chamber of the heart), making it difficult for enough blood to be pumped into the body. This blockage can result in strain on the left ventricle since it is working harder than normal to pump blood. Eventually, it can also cause damage to the aortic valve.
On June 12, 2013, a few weeks after her first birthday, Kennedy underwent surgery to address the stenosis. The surgery was performed by Dr. Timothy Pettitt, pediatric cardiothoracic surgeon at Children’s Hospital New Orleans.
“To address subaortic stenosis, we perform an operation called a subaortic resection, in which we make a vertical incision in the middle of the chest and typically need to place the patient on a heart-lung bypass machine,” Dr. Pettitt said. “We then perform the repair by opening the aorta, just above the aortic valve, and then cut the membrane out, which opens the left ventricle’s outflow track. This results in a more even flow of blood and preserves the function of the left ventricle. If left alone, that ventricle will work progressively harder and would eventually lead to enlargement of the heart and possibly heart failure.”
The surgery was successful and Kennedy’s recovery was faster than expected.
“She was so strong and amazed everyone by how quickly she recovered,” Kim said. “Meanwhile, we were just so happy with the team and everyone at the hospital from the very beginning. The entire team, from the surgeons to the nurses in the CICU, were phenomenal—they were just the most compassionate people, and I cannot speak highly enough of them.”
 Kennedy’s post-surgery prognosis was positive, with a nearly 80% chance that her membrane would not regrow. Her heart condition is rare, however, and it is typically seen alongside other defects. But after extensive tests, including in-depth genetic testing, her specialists could not determine any other abnormality.
Kennedy’s post-surgery prognosis was positive, with a nearly 80% chance that her membrane would not regrow. Her heart condition is rare, however, and it is typically seen alongside other defects. But after extensive tests, including in-depth genetic testing, her specialists could not determine any other abnormality.
“The geneticist explained that more than likely, Kyle and I both had some genetic wildcards and together, they may have contributed to this,” Kim said.
As the months went by, Kennedy grew bigger and stronger, and her heart was regularly checked during routine appointments with her cardiologists. A little over one year after her first surgery, however, her doctors told Kim and Kyle that her membrane was beginning to regrow progressively.
“By the time she was 3, we were beginning to prepare for another surgery,” Kim said.
But then, something miraculous happened.
During a routine echocardiogram one day, the technician was taking much longer than usual to complete the measurements.
“We were sitting there for an hour and a half, and we finally started to panic,” Kim said. “I was watching the screen, and I had gotten to the point where I was familiar with what we would see during each appointment. I turned to Kyle and I said, ‘I don’t know what the problem is, I don’t see anything.’”
Finally, the cardiologist came in and took over. She spent another 30 minutes performing the test.
“After what seemed like forever, she turned off the screen and looked at us and said, ‘I have no way of explaining why we are seeing this, but Kennedy’s membrane has decreased significantly.’”
A wave of relief swept over Kim and Kyle, who understood this meant they could postpone the surgery. Their prayers had been answered by this unexpected improvement, and the couple felt confident that the road ahead for their daughter was about to get much easier.
 And for a while, it was. Kennedy started school and was met with new challenges, some related to her speech and her vision, but she handled each with courage and perseverance. She enjoyed making friends and loved learning. She also continued to see her local cardiologist, and as the years went by, her membrane slowly began to grow back.
And for a while, it was. Kennedy started school and was met with new challenges, some related to her speech and her vision, but she handled each with courage and perseverance. She enjoyed making friends and loved learning. She also continued to see her local cardiologist, and as the years went by, her membrane slowly began to grow back.
In 2019, she was once again referred to Children’s Hospital New Orleans. During one of their initial visits, her doctor explained to the Lords that Kennedy’s membrane was growing to the point that it was starting to effect other aspects of her heart. He also told them that after he reviewed her health history, including years of echocardiograms, he observed that there was a progressive deficiency with her aortic valve, which is a known side effect of subaortic stenosis.
The inconsistent blood flow from the left ventricle can eventually cause damage to the aortic valve, which results in leakage and needs to be addressed. This is common in patients with subaortic stenosis, and in Kennedy’s case, her growing membrane was directly affecting the function of her aortic valve, and without surgery, it was only going to get worse. The news was devastating, but the Lords understood that there was no other option.
“At this point, we were no longer just talking about a subaortic membrane repair, but also an even more complex open-heart surgery,” Kim said.
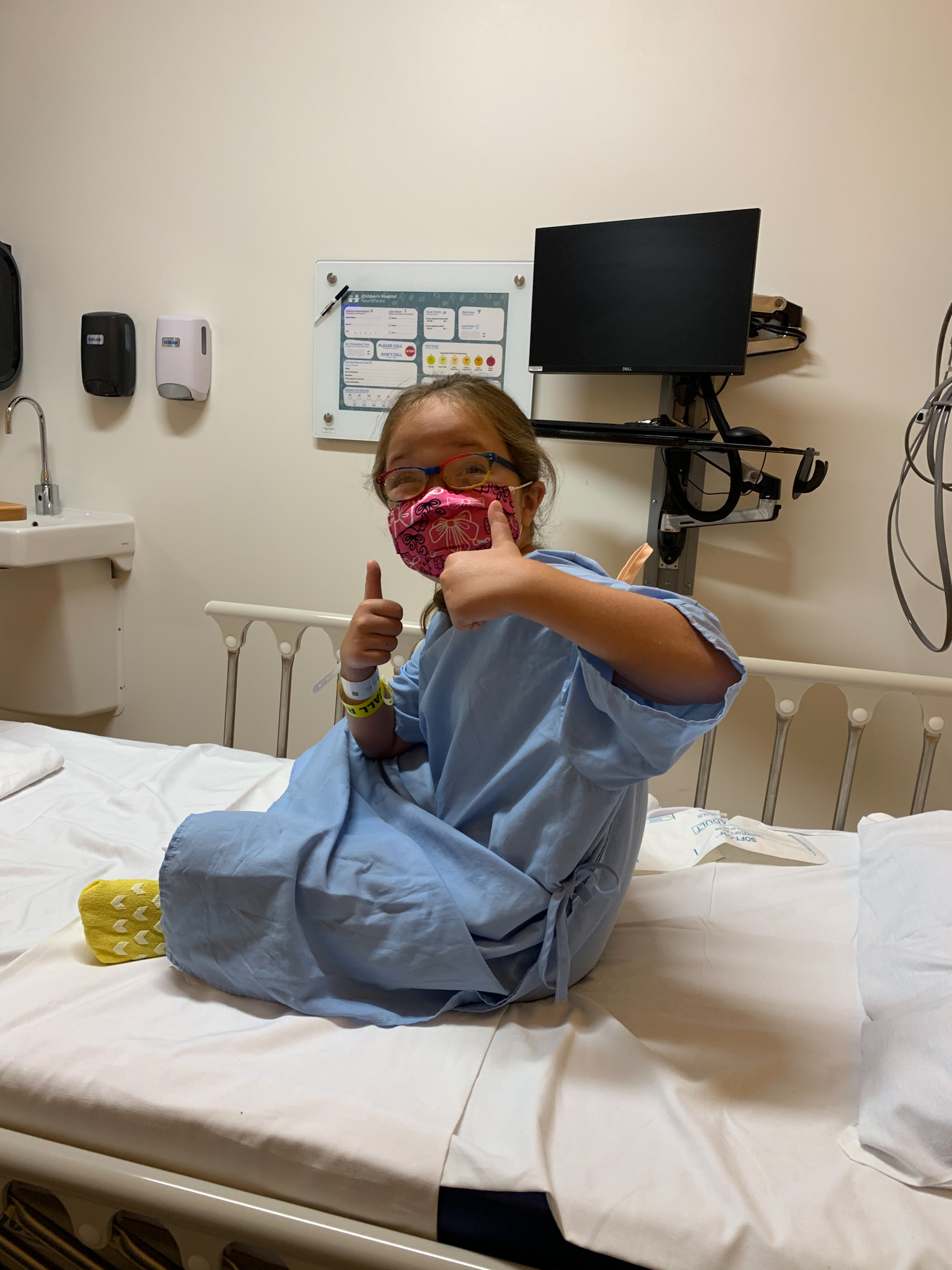
Kennedy's cardiologist worked closely with Dr. Pettitt to develop a plan for the surgery, which was scheduled for July 14, 2020. It would be a multi-step process and a complex procedure that would include a resection of the membrane and also a repair to the aortic valve. Kennedy, now 8 years old and headed into the third grade, summoned all of her courage ahead of that day.
All-in-all, the surgery took more than 10 hours. In addition to removing the membrane once again, Dr. Pettitt performed what is known as the Ross procedure, which involves replacing the damaged aortic valve with the pulmonary valve.
“We utilize the Ross procedure when a patient’s aortic valve is severely damaged,” Dr. Pettitt said. “This involves surgically replacing the diseased aortic valve with the patient’s pulmonary valve, and then replacing that pulmonary valve with a healthy donor valve or allograft. This is a highly specialized and complex open-heart surgery, but it allows patients with diseased aortic valves an excellent prognosis.”
 Because the surgery took place in the middle of the COVID-19 pandemic, the hospital had strict visitation rules. Kim said she and Kyle will forever be thankful for the opportunity to stay at Hogs House during Kennedy’s surgery, an on-campus housing facility supported by the organization Hogs for the Cause, which provides a place for families who live outside New Orleans to stay while their child receives ongoing care at the hospital.
Because the surgery took place in the middle of the COVID-19 pandemic, the hospital had strict visitation rules. Kim said she and Kyle will forever be thankful for the opportunity to stay at Hogs House during Kennedy’s surgery, an on-campus housing facility supported by the organization Hogs for the Cause, which provides a place for families who live outside New Orleans to stay while their child receives ongoing care at the hospital.
“It was such a blessing, because we couldn’t stay in the waiting room because of the COVID-19 protocols,” Kim said. “The medical team was wonderful, too. They kept us updated regularly throughout the surgery, and then as Kennedy was recovering, there was a nurse that literally watched her every moment for about 14 hours until they removed her breathing tube. They did not take their eyes off her, and it was the most amazing and comforting thing for me as a mother who couldn’t stay in the room with her during that time.”
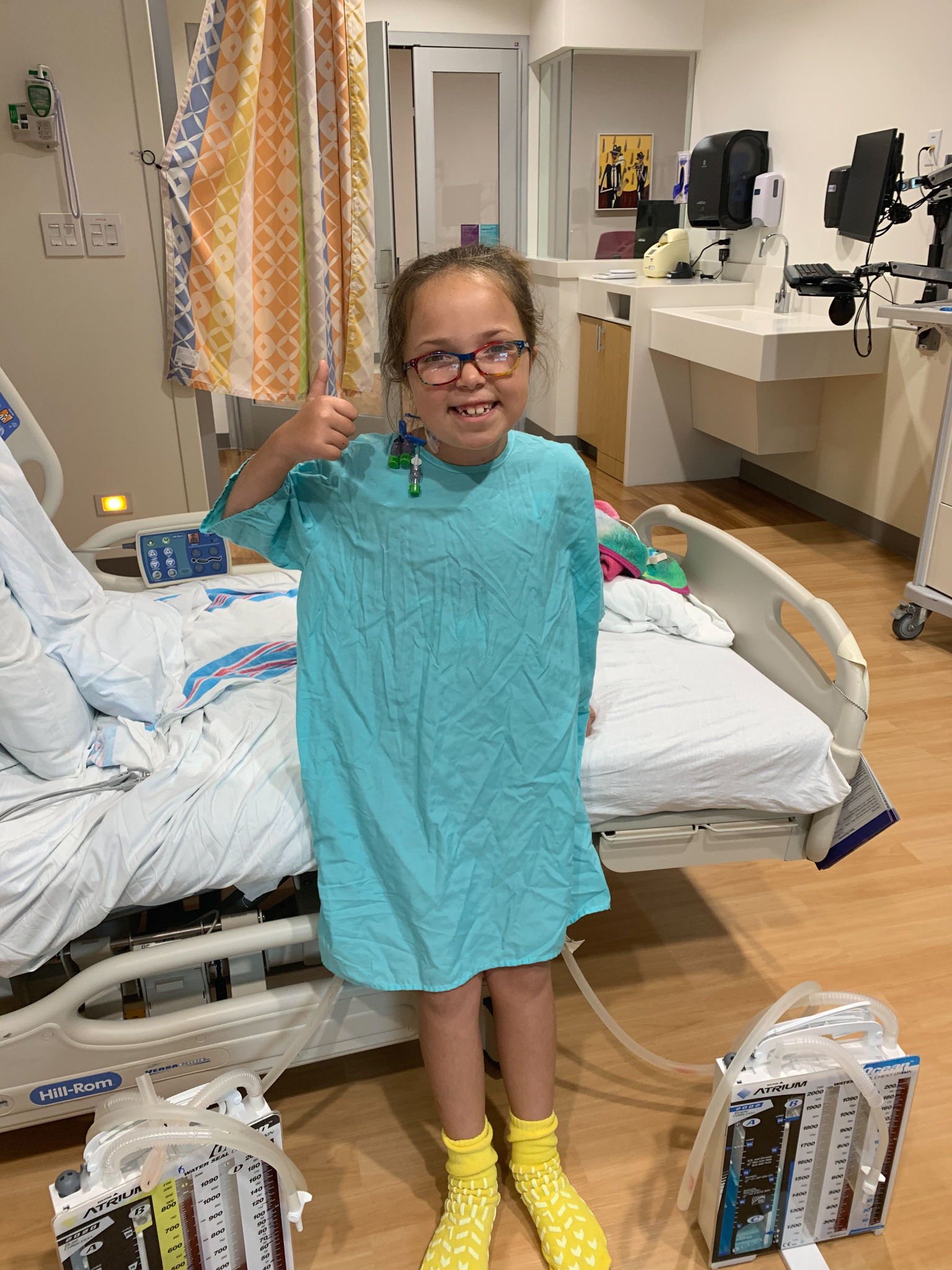
Just as she did when she was a baby, Kennedy impressed everyone with her determination and strength during her road to recovery. The medical team had scheduled her to be at the hospital for 14 days, but on day 5, she was already ready to be discharged.
“She was such a trooper, and she continues to be,” Kim said. “Her heart is doing beautifully now, but she will need to be monitored for the rest of her life, and we don’t know what the future looks like in terms of additional surgeries. Her membrane may grow back and her valve will always have some issues, but overall, she is doing so well.”
 Today, Kennedy is thriving. Now in the fifth grade, she is a whiz at math, and a member of the cheerleading squad and the student council.
Today, Kennedy is thriving. Now in the fifth grade, she is a whiz at math, and a member of the cheerleading squad and the student council.
“Looking at her, you would never know that she’s had these issues with her heart,” Kim said. “If you didn’t see the scar on her chest, you would have no clue that she has been through what she has been through. On top of everything, she is a super compassionate kid who will go out of her way to help someone feel like they belong. This is the way God made her, and we are so blessed.”
To learn more about the Heart Center at Children’s Hospital New Orleans, visit https://www.chnola.org/our-services/heart-center/



