My ray of sunshine: Norah’s miraculous journey after being diagnosed with a one-of-a-kind genetic disorder
- Category: Cardiology, General Health, Living Well, Orthopedics
- Posted on:

When Chrissy Solice found out she was expecting her second daughter, she never imagined her baby’s journey would be an uphill battle. After surviving 14 surgeries and an undiagnosed genetic disorder that caused her numerous health issues, Chrissy’s 5-year-old daughter, Norah, has taught her many things: to never lose hope no matter what life throws at you and to cherish every moment with each other.
“No diagnosis – no matter how scary it sounded - could ever change the way I felt about the beautiful blessing God had given me,” said Chrissy. “To me, my daughter was perfect, even though we knew something could be genetically wrong with her. When I was 20-weeks pregnant, I found out Norah had a single umbilical artery. My OB/GYN was concerned because a missing artery in the umbilical cord could lead to an increased risk of heart and kidney problem, since these organs usually develop at the same time. I began seeing a high-risk maternal fetal medicine (MFM) physician to monitor my pregnancy closely.”
Despite having a single umbilical artery, Norah’s fetal scans and echocardiograms, an ultrasound of the heart, showed her heart and kidneys were doing well, but her growth and development were lagging. Since she was on the smaller end of the scale, her doctors monitored her growth often. Chrissy also had bi-weekly stress tests.
When Chrissy was 25 weeks along, she learned her daughter’s growth had slowed down and she was placed on bedrest for 10 weeks. Her doctors thought Norah wasn’t getting enough nutrition due to her single umbilical artery. As they monitored her growth each week, Norah was still growing and was very active in her mother’s womb. When Chrissy went in for her daughter’s 35-week ultrasound, her MFM physician noticed Norah’s growth dropped below three percent. At this point, the risks were too high if she remained in her mother’s womb. That same day – on Dec. 21, 2016 - Chrissy was admitted to Slidell Memorial Hospital. When she arrived, she was induced immediately.
“I was having contractions, but Norah hadn’t dropped,” said Chrissy. “My doctor thought she was too little and couldn’t put pressure on my cervix to move things forward. The next day, Norah’s heart rate dropped. It was scary. Initially, they put me on oxygen to see if that improved the situation, but Norah’s heart rate dropped again. I ended up having a C-section. I was thankful my sister was with me in the delivery room. Norah was born on December 22 and weighed 3 pounds, 12 ounces. After she was born, instead of cheers, I heard total silence in the room. The doctor asked me, ‘Did we do genetic testing on her? And I said yes.’ After they intubated her, I could still feel an uncomfortable heaviness in the room.”
While Chrissy recovered from her C-section, Norah was transported to the neonatal intensive care unit (NICU) for further observation. As they examined Norah, her NICU doctors treated her for a collapsed lung. They also suspected Norah had a genetic abnormality because she had unusual physical characteristics. Her neck was wide, her ears were low set, and her eyes were widespread. Her toes were webbed, and her pinkies were a little curved. Chrissy was told her baby, who was 18-hours old, would be transferred to Children’s Hospital New Orleans where she would require a higher level of NICU care.
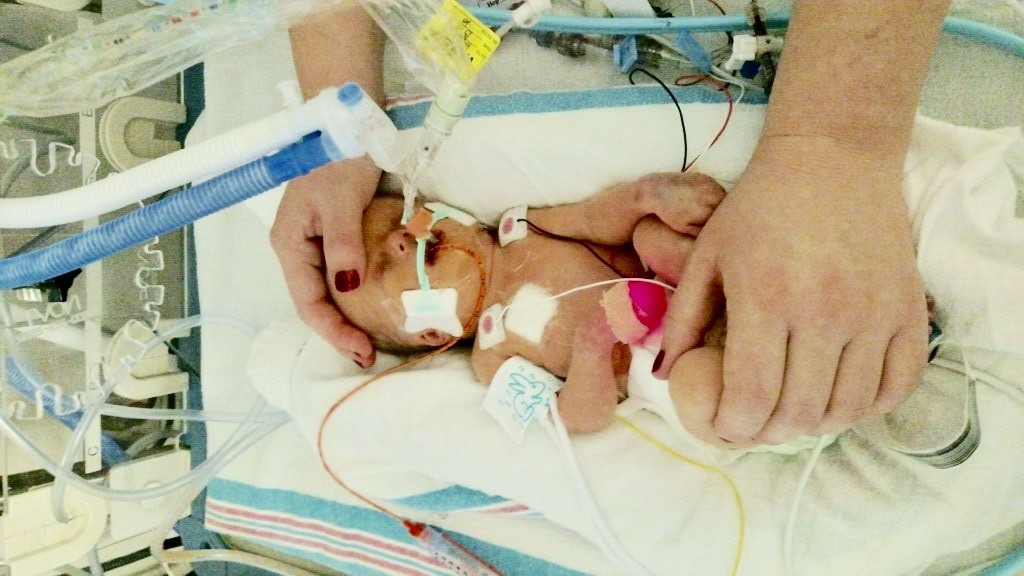
“When my sister showed me photos of Norah in the NICU, I thought I’d see this little warm pink bundle,” said Chrissy. “Instead, every inch of her body was covered in tubes and wires. I cried. I was exhausted and didn’t sleep that night. I was afraid if I fell asleep, I would wake up and find Norah gone. There were so many things that confused me about Norah’s condition. We knew this baby from head to toe. We had fetal scans done on her. We had gone over her with a fine-tooth comb for many months. We knew she was going to be small, but little did we know, she would have many health problems that nobody saw coming. I remember the transport team preparing Norah for the 17-minute helicopter ride to Children’s Hospital. Before they departed, they wheeled her in my room. That was the first time I laid eyes on my baby. I had a couple seconds with her and then it was time for her to leave. I said hello and goodbye to her for the first time. It was a sad moment, but I knew she would be in good hands at Children’s Hospital.” 
Later that evening, Norah’s cardiologist, Dr. Christian Lilje told Chrissy that her daughter had multiple congenital heart defects. She had an interrupted aortic arch type B, a condition where her aorta did not develop properly. She had a large ventricular septal defect, a hole in the wall that separates the heart's lower chambers, and a bicuspid valve in which two of the leaflets of the aortic valve fused together during fetal development resulting in a two-leaflet valve instead of a three-leaflet valve. If left untreated, these problems could lead to heart failure. Alongside these diagnoses, Norah had a patent ductus arteriosus (PDA). This opening supplies oxygen-rich blood to the lower half of a baby’s body in utero but naturally closes shortly after birth. In Norah’s case, her PDA stayed open which turned out to be a good thing. If her PDA closed, she would have gone into shock and died. She was given prostaglandin to keep the PDA open until her surgery. She had two pulse oxygen probes to monitor her oxygen levels. Her cardiology team knew if oxygenated blood was flowing to her lower body, it was a sign her PDA was still open.
“It was heart-breaking to hear about my daughter’s condition,” said Chrissy. “The tough part was finding out about everything by phone since I was still recovering from my C-section at Slidell Memorial. After I was released from the hospital on Christmas Eve, I rushed to the NICU to spend time with my daughter. Still, there were so many emotions racing through my mind. I was extremely scared and overwhelmed, and uncertain if my daughter would survive this. I was grateful to have my 10-year-old daughter, Lena, with me and the support from our family and friends. As a single mother, I couldn’t do this without them.”
On January 4, 2017, Norah had her first “hybrid” heart surgery when she was 2 weeks old, performed by Drs. Ernest Siwik, Kiran Mallula, Joseph Caspi, and Timothy Pettitt. This procedure included both a heart surgery to place pulmonary artery bands and a heart catheterization to insert a stent in her PDA to keep it open. After her surgery, Norah’s lungs started to improve, her bleed on her adrenal gland cleared up, and her stomach issues resolved.
Then, a few days later, the results from Norah’s first round of chromosomal microarray testing came back. Norah had a genetic condition her doctors had never documented before. A third copy of the long arm of her seventh chromosome was stuck on her twenty-second chromosome. It was a very large chromosomal duplication that impacted 589 genes. Because her doctors didn’t know much about this defect since Norah was the only person who had it, they assumed that any medical condition she was diagnosed with might be connected to this large duplication. All her organ systems were being affected in one way or another.
“The stent in her PDA was only supposed to last for about four to six months before she got her full heart repair surgery,” said Chrissy. “The stent surgery gave her time to grow. We knew we were on borrowed time before she got her next heart surgery. Besides her heart issues, my daughter had a cluster of other problems that affected multiple organ systems. When Norah was 2 months old, she had trach and G-tube placement. Then, a few weeks later, she developed necrotizing enterocolitis, a life-threatening intestinal inflammation. Since this condition was caught early, she was treated with antibiotics. She also developed hydrocephalus (brain swelling) that eventually required shunt placement surgery. Norah had brain bleeds that happened spontaneously. When we got her checked out, we learned she had an undiagnosed platelet disorder. Norah spent five months in the NICU before we could take her home.”
In June 2017, Dr. Oritjejolomi Roberts performed Norah’s shunt placement surgery for hydrocephalus. A month later, she had her shunt replaced due to a blood clot that formed in the shunt. After undergoing her third shunt revision surgery in November 2017, Norah didn’t have any more brain swelling. A year after Norah’s first open-heart surgery, her multidisciplinary team prepared for her second heart surgery.
“Norah was the longest hybrid that had ever been at Children’s Hospital,” said Chrissy. “That was the longest span of time between her first and second heart surgery. Once we found out she had a platelet disorder, her doctors were cautious about how to proceed with her heart surgery. Her doctors prepared for possible scenarios that could happen during the procedure. I was included in a multidisciplinary meeting where I met with all the doctors from neurology, neurosurgery, hematology, cardiology, and cardiac surgery. We sat around a table and weighed our options. Norah had a 60 percent chance of making it through the surgery. There was also a large chance of Norah having a catastrophic brain bleed during the surgery. But without surgery, my option was to take her home and pretty much love on her until she passed. Dr. Pettitt performed her 12-hour surgery. He struggled to get her bleeding under control. It took five hours to get it under control, but her heart was repaired. She came back to the CICU with her chest open. Seeing her heart beating was the most beautiful thing I had ever seen. We left the hospital a month later. She was pinker than ever. Aside from the fact she had a vent trach, she was doing great after her second heart surgery. With her heart and brain problems under control, I thought nothing was stopping her now from living. So, I started feeling more optimistic about the future.”
Three months after her surgery, she was hospitalized for another bout of necrotizing enterocolitis. She was on IV antibiotics, but her veins were weak, so her doctors put her on a central line. At one point, the surgeon told Chrissy we really need to think long and hard before pulling the line because that could be the last line she will ever have. At that point, Chrissy thought, “This can’t be happening. She has been through so much and she has done so well. Is this how she goes out over not being able to get an IV?” 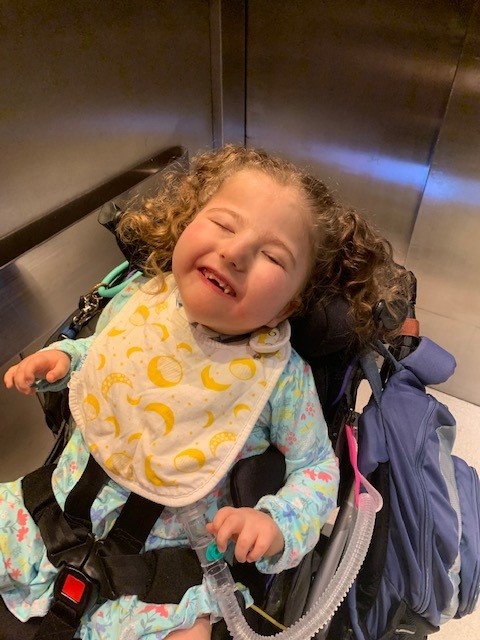
“That’s when we began working with the Pelican Crew, the palliative care team at Children’s Hospital,” said Chrissy. “They were amazing. They brought together different disciplines during Norah’s hospital stay. I soon realized they are all about comfort, not just end-of-life care that I automatically associated with, ‘palliative care.’ It was more about what they could do to make Norah’s life as good as possible. They brought in music therapy and helped line up services to make Norah’s stay more enjoyable. The biggest thing is they listened to what I wanted for my daughter. They were a wonderful support system.”
Although Norah had a few more health issues over the years – 11 kidney infections, bladder surgeries, severe scoliosis, a diagnosis of epilepsy, and craniosynostosis where sutures in her brain and skull closed prematurely – Chrissy says her beautiful 5-year-old daughter would not be here today if it weren’t for the wonderful multidisciplinary team (from neurology, cardiology, genetics, endocrine, nephrology, pulmonology, hematology, neurosurgery, ENT, respiratory, GI, and orthopedics) who took care of her like she was their own. She will continue regular follow-ups with these services including regular follow-up for her heart conditions with her cardiologist, Dr. Kelly Gajewski.
“When I hand her over to the team at Children’s Hospital for care I’m not handing her over to just doctors or nurses, I’m handing her over to family. They are the family that I thought I would never have, but absolutely needed,” said Chrissy. Everybody knows my daughter’s name and continues to be her biggest cheerleaders. She is Children’s Hospital’s baby. The nurses at the hospital have been strong advocates for her. They supported me when I was in the NICU with her and throughout our journey. They made sure I was getting enough food and rest. They always wanted to make sure my daughter and I were comfortable, and they met our every need. The doctors have been like therapists to me, especially Dr. Christian and Dr. Roberts, who I call my friends. They listened to me and valued my input. They were always attentive to my concerns and encouraged me to follow my motherly instinct. The respiratory team was amazing, too! They taught me everything I needed to know about trach care before Norah came home from the hospital. I realized I was more prepared than I thought I was. There is nowhere else I would have taken my daughter for her care. This is where she started her journey, and this is where she continues her journey. She’s had three life-flights, so I am really a big fan of the transport team. Children’s Hospital will always have a special place in my heart.”
Chrissy and her 15-year-old daughter Lena consider every day with Norah a blessing. Chrissy says her dream for Norah is to give her the absolute best life possible while keeping her comfortable and happy.
“Life is precious, and my family and I cherish every single moment with her,” said Chrissy. “Norah is our miracle and little ray of sunshine. Even though I sometimes feel like I’m on borrowed time, my goal is to make every step of her journey as happy and fulfilling as possible. I want her to be loved and feel loved.”
To learn more about the services available at Children’s New Orleans, please visit: https://www.chnola.org/ 



